When basic instincts take a beating
As addiction to drugs and alcohol climbs new highs in India, it is essential to treat the condition through a multifaceted approach
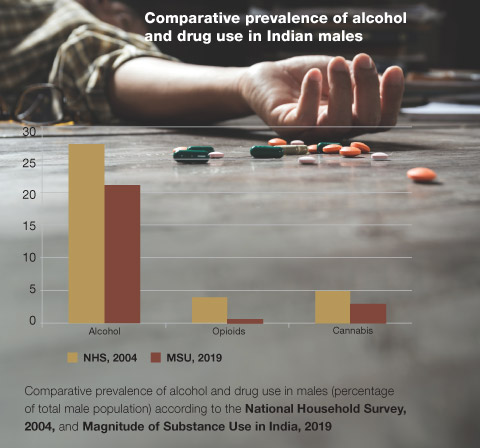
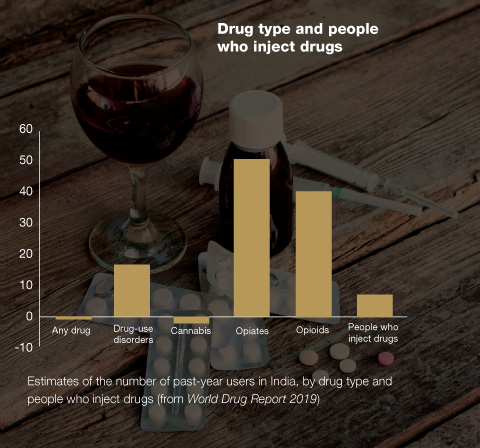
The statistics are staggering and cause for alarm. According to a recently conducted nationwide survey, nearly 57 million people in India are estimated to be impaired by alcoholism and need treatment. Nearly 8 million people are affected by opioids such as heroin and opium and by drugs such as codeine, dextropropoxyphene, diphenoxylate and buprenorphine.
Natural opioids, which once dominated the scene, have been replaced by heroin and pharmaceutical drugs. High-risk patterns of opioid use — injection and the sharing and reusing of needles and syringes — are on the rise, increasing the risks of overdose and blood-borne infections. There is wide variation in drug and alcohol use across India’s states, which could be attributed to sociocultural, economic and geographical differences. In some states the problem of drug addiction is endemic.

The cost to society is equally staggering. People in their prime years, between 17 and 55, are hit the worst and we could potentially lose a generation to the addiction problem. The Global Burden of Disease (2016) study estimated that mortality due to drug use disorders peaks before age 40. Alcohol is not a lesser evil. The Global Status Report on Alcohol & Heath reported that 5.3% of global deaths are related to alcohol use.
This is more than the combined death toll attributed to tuberculosis, diabetes and Aids. Direct costs related to health, infections, accidents and hospitalisation run into thousands of crores and indirect costs from diminished productivity, job loss, absenteeism, and law and order problems are about as high.
Addictive disorders should be viewed as a non-infective epidemic. The ‘pathogens’ are drugs and alcohol and the two major factors spreading the ‘contagion’ are supply, or access, and price. If supply is plentiful and the price low, the epidemic spreads and makes treatment challenging.

Percy Menzies
is the president of Assisted Recovery Centres of America, a medical treatment facility for alcohol and drug use disorders based in St Louis, Missouri, USA.
Addictions are often described as chronic, progressive conditions, much like hypertension, asthma or diabetes. There may be some similarities but there are radical differences. Addictions impact the basic survival instincts so essential for life. Humans are endowed with a ‘mind’, or the thinking brain, that controls the primordial brain involved in survival. The intricate dynamic between mind and brain is essential for thriving.
Humans are created to thrive, not survive. Addictions disrupt this critical balance and throw patients into survival mode, a dangerous state to be in. The brain is tricked into believing that the only thing needed to survive is the drug or the alcohol. The aspects of thriving — jobs, family, personal safety and behaviours — have little or no relevance. There are no rules of engagement. Do whatever it takes to survive. Lie, cheat, steal, sell your body to obtain the drug or alcohol to feel ‘normal’.

Abhishek Ghosh
is an assistant professor at the Postgraduate Institute of Medical Education & Research, Chandigarh.
Punishment trap
Over time this behaviour gets entrenched and becomes an obstacle to long-term recovery. Obviously, such behaviours have no place in society and the common reaction to bring about change is punishment and stigma.
Repeated bouts of punishment, like arrest, jail and unproven ‘treatments’, don’t work and patients relapse quickly. This has often led to the conclusion that addiction is an ‘incurable disease’, one that is best treated through the criminal justice system or through self-help and spiritual groups.
Why do patients relapse despite the trauma and pain to themselves and their families? We must look again at how fundamentally different addiction is from other chronic conditions. Addiction impacts the basic instincts of survival by getting embedded in the memory, motivational and emotional circuits of the brain. It is driven by conditioning and reinforced by cues and triggers.
The cues most often associated with addiction are sights, sounds, places, people and the time of day associated with drug or alcohol use.
There is the misconception that taking patients away from the cues and triggers will cure them. The widely used treatment model is to send the patient away for 28 days or longer to a residential facility where they have minimal exposure to myriad cues and triggers. Patients and their families may feel good for a while and get their hopes up for a cure.
This well-studied phenomenon is called the ‘deprivation effect’. In the simplest of terms, the longer the patient is deprived of his/her favourite high, the stronger the desire to use when access is restored. We have not found a strategy to curtail or cut off the supply of drugs and alcohol, making relapse prevention considerably difficult.
Hope still shines
Is there hope for patients to get well? The answer is a resounding ‘yes’. Advances in the fields of neuroscience and behavioural science have led to the development of highly effective medication to treat addictions, and behavioural therapies to help patients regain their lives. India is fortunate to have access to such medications and therapies. However, the treatment gap in the country is enormous.
Among mental illnesses, alcohol-use disorders have the highest treatment gap — nearly 90%, which means only one in ten people with problematic alcohol use seek medical help. For drug-use disorders, barely 25% of patients seek any type of professional help.
The reasons for this could be summarised by the 4 ‘As’: lack of ‘availability’ of treatment centres delivering evidence-based care; poor ‘accessibility’ because of services being concentrated in cities; less ‘affordable’ care due to the small numbers of publicly funded treatment facilities; and poor ‘awareness’ of addiction as a treatable medical disorder. There are silver linings, though, such as the Mental Health Care Act (2017), which termed addiction as a mental illness and promised patients the right to publicly funded healthcare.
India scenario
Unlike Western countries, in India most patients affected by drugs and alcohol have family support. Addiction is often described as a family disorder. It impacts the entire family and, as such, treatment should involve family members. They can play a key role in bringing patients to the clinic, in ensuring that they take anti-craving medication, and in providing the emotional and spiritual support so essential in recovery.
The treatment of addictions is not complex and does not require sophisticated and expensive devices and equipment. What it requires is a multifaceted approach involving physicians, nurses, therapists, social workers and family members. By the time the patient seeks treatment, the needs are multidimensional. They are likely to have medical and psychiatric problems, along with legal, marital, financial and employment issues.
Each of these challenges need to be addressed to prevent the patient sliding into relapse. It may take several attempts before the patient fully recovers. A good example is helping patients quit smoking. Few quit at the first attempt, but every slip becomes an opportunity to work harder and smarter and finally achieve the goal of recovery. This debunks the myth that addiction is incurable.
The views expressed are those of the author and do not reflect the official policy or position of the Tata Trusts.
